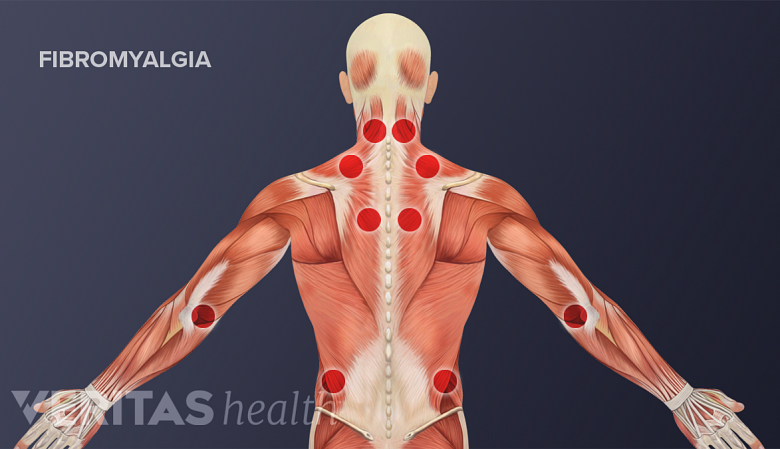
Fibromyalgia is a fairly common syndrome characterized by symptoms such as muscle pain, painful areas of the body called tender points, and fatigue.
Fibromyalgia causes fatigue and pain in tender points of the muscles.
The overall extent and nature of symptoms vary widely from person to person, and the symptoms may be chronic or they may come and go over time, sometimes making it challenging to get an accurate diagnosis.
In This Article:
- What You Need to Know About Fibromyalgia
- Characteristic Symptoms of Fibromyalgia
- How to Get a Fibromyalgia Diagnosis
- Multi-Specialty Fibromyalgia Treatment
- Medications to Ease Fibromyalgia Symptoms
The term fibromyalgia stems from the Latin “fibra,” for fibrous tissue, the Greek words “mys” for muscle, and “algia” for pain. Before the 1980s, the condition was called fibrositis.
Fibromyalgia does not harm organs and is almost never life-threatening, though it can significantly impact one's quality of life. The focus of treatment is to manage the pain and symptoms.
Rheumatic Condition
Fibromyalgia shares some symptoms with arthritis, including chronic pain and fatigue. Like arthritis, it is considered a rheumatic condition because it has an impact on the muscles, joints, and bones. The condition is different from chronic pain and arthritis in important ways, however, such as:
- Fibromyalgia does not damage joints or muscles, and inflammation does not play a significant role, though many of the tender points are near the joints.
- There are no outward signs of inflammation in adults. Children may experience some brief swelling.
- Fibromyalgia is not a degenerative condition. Patients’ symptoms may improve following diagnosis and treatment.
Rheumatologists often treat fibromyalgia, but many people also see internists, family practice physicians or other qualified health professionals to manage their condition.
Due to the range of symptoms associated with fibromyalgia, an interdisciplinary health care team is generally beneficial. In addition to the main treating physician, who is usually a rheumatologist, a physical therapist is usually part of this team, and a chiropractor, neurologist, pain specialist, physiatrist, and psychologist or psychiatrist may also be involved.
Coexisting Conditions
Many individuals with fibromyalgia have at least one other medical condition.
See Fibromyalgia or Not? 6 Conditions to Know
Other rheumatic conditions are especially common in those with fibromyalgia. An estimated 25% to 65% also have systemic lupus erythematosus, ankylosing spondylitis, or rheumatoid arthritis.
Symptoms of these coexisting conditions may overlap with those of fibromyalgia, leading to a delay in diagnosis. Further complicating a diagnosis is the fact that there is no single, widely accepted diagnostic test for fibromyalgia. Instead, diagnosis is based largely on the patient's symptoms and by using medical tests to rule out other conditions.
See Rheumatoid Arthritis (RA) Diagnosis
Cause Is Unknown
When an individual has fibromyalgia, the brain overreacts to pain signals, intensifying feelings of pain in different parts of the body. It is not known what sets off this reaction, though in some cases it appears to be tied to a stressful or traumatic event, illness, injury, or another disease. The condition runs in families, but a specific gene for fibromyalgia has not been found.
More Common in Women
It is estimated that about 2% to 4% of adults have fibromyalgia. 1 Fibromyalgia: Fast Facts, American College of Rheumatology. Fibromyalgia. About 80% to 90% of people with fibromyalgia are women, 1 Fibromyalgia: Fast Facts, American College of Rheumatology. Fibromyalgia. typically between the ages of 40 and 75, and the symptoms tend to be more severe in women.
In recent years, more men have been diagnosed than in the past, possibly as a result of shifts in the diagnostic criteria beginning in 2010. 2 Vincent A, Lahr BD, Wolfe F, et al. Prevalence of fibromyalgia: a population-based study in Olmsted County, Minnesota, utilizing the Rochester Epidemiology Project. Arthritis Care Res (Hoboken). 2013;65(5):786-92. , 3 Bennett RM, Friend R, Marcus D, et al. Criteria for the diagnosis of fibromyalgia: validation of the modified 2010 preliminary American College of Rheumatology criteria and the development of alternative criteria. Arthritis Care Res (Hoboken). 2014;66(9):1364-73. In children, the condition is most often diagnosed in adolescence and is known as juvenile-onset fibromyalgia.
See Symptoms and Causes of Juvenile Rheumatologic Diseases
Under-diagnosis is a major concern; it is believed that up to 75 percent of those with fibromyalgia have not been diagnosed. 4 Clauw DJ, Arnold LM, Mccarberg BH. The science of fibromyalgia. Mayo Clin Proc. 2011;86(9):907-11.
- 1 Fibromyalgia: Fast Facts, American College of Rheumatology. Fibromyalgia.
- 2 Vincent A, Lahr BD, Wolfe F, et al. Prevalence of fibromyalgia: a population-based study in Olmsted County, Minnesota, utilizing the Rochester Epidemiology Project. Arthritis Care Res (Hoboken). 2013;65(5):786-92.
- 3 Bennett RM, Friend R, Marcus D, et al. Criteria for the diagnosis of fibromyalgia: validation of the modified 2010 preliminary American College of Rheumatology criteria and the development of alternative criteria. Arthritis Care Res (Hoboken). 2014;66(9):1364-73.
- 4 Clauw DJ, Arnold LM, Mccarberg BH. The science of fibromyalgia. Mayo Clin Proc. 2011;86(9):907-11.