The symptoms of polymyalgia rheumatica (PMR) can come on quite suddenly or more insidiously.
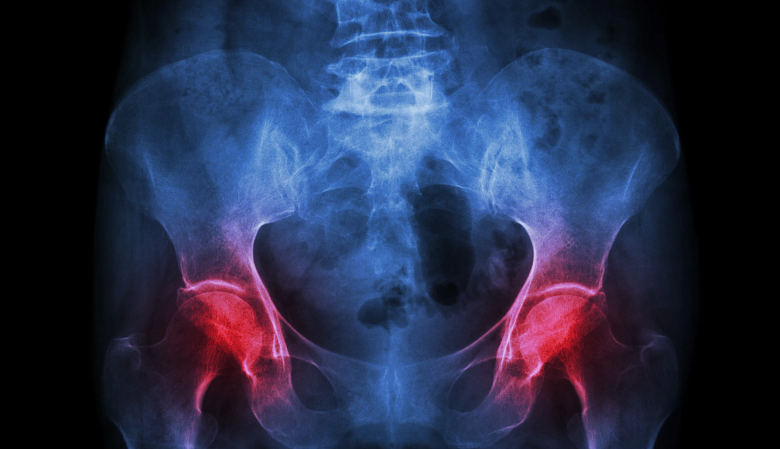
Pain from polymyalgia rheumatica often affects both sides of the hips or shoulders at once.
In This Article:
Physical Symptoms of PMR
The common physical symptoms of PMR are listed below.
- Severe pain usually starts in the shoulders and is typically described as a muscle ache similar to a flu or vigorous exercise. The pain may gradually spread over to the neck and hip regions.
- Symmetrical joint pain is commonly seen in PMR affecting both the right and left sides (for example, both shoulders or both hips).
- Morning stiffness lasting for hours is a common symptom of PMR. Stiffening of joints due to immobility, or long periods of resting can also occur later in the day. In severe cases, the stiffness may last for an entire day.
- Difficulty in performing daily activities, such as rising from bed, walking, or raising arms to comb hair is common. Climbing stairs or getting in or out of a car can also be painful.
- Pain at night is seen in some cases. This pain is typically most severe between 4 am and 6 am, causing disturbed sleep. 1 Mandell BF. Polymyalgia rheumatica: Clinical presentation is key to diagnosis and treatment. Cleve Clin J Med 2004; 71 : 489-95. And Mackie SL, Hughes R, Walsh M, Day J, Newton M, Pease C, et al. "An impediment to living life": Why and how should we measure stiffness in polymyalgia rheumatica? PLoS One 2015; 10 : e0126758. As cited in - Milchert M, Brzosko M. Diagnosis of polymyalgia rheumatica usually means a favourable outcome for your patient. Indian Journal Of Medical Research [serial online]. May 2017;145(5):593-600.
- A low-grade fever and muscle aches may be present from the start of the symptoms and last for more than a month.
- A general feeling of tiredness or being unwell may resemble having a flu that lasts for weeks and maybe even for months.
Several of the above-mentioned symptoms may be seen in the early stages of PMR.
Other symptoms of PMR may appear later as the inflammation in the joints worsen, including:
- Decreased appetite leading to weight loss
- Swelling and fluid accumulation causing pitting edema or swelling without pitting edema (Pitting edema is characterized by applying pressure with a finger on the swollen area, creating a depression—the skin and underlying tissue do not quickly bounce back)
Most people with PMR, especially those in good health before their symptoms, may feel overwhelmed due to its sudden appearance and impact on everyday life.
Rarely, PMR may cause symptoms that are not very characteristic of the condition, such as:
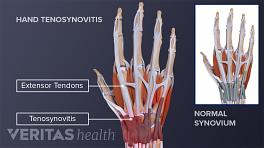
- Carpal tunnel syndrome
- Pain in the knees, wrists, and hands affecting only one side
See Carpal Tunnel Syndrome Video
Specifically identifying and describing symptoms of PMR can help lead to an accurate diagnosis.
Emotional Symptoms of PMR
PMR can have an adverse effect on mental health. For example, people who have PMR may experience:
- Depression resulting from loss of physical activity
- Low self-esteem due to sudden loss of weight
- A sudden decline in physical well-being, leading to the feeling of aging faster
It is advisable to consult a doctor or mental health counselor if feelings of depression or low self-esteem are experienced.
Association with Giant Cell Arteritis
Giant cell arteritis or temporal arteritis has been noted to occur alongside PMR in many cases. Some of the common symptoms of giant cell arteritis include:
- Visual disturbances
- Inflammation of blood vessels in the scalp, resulting in headaches
- Pain in the jaw while chewing
If left untreated, giant cell arteritis can lead to permanent blindness. 2 Diamantopoulos AP, Haugeberg G, Lindland A, Myklebust G. The fast-track ultrasound clinic for early diagnosis of giant cell arteritis significantly reduces permanent visual impairment: towards a more effective strategy to improve clinical outcome in giant cell arteritis?. Rheumatology (Oxford). 2016;55(1):66-70. If vision problems are experienced after being diagnosed with PMR, it is advisable to seek immediate medical attention.
- 1 Mandell BF. Polymyalgia rheumatica: Clinical presentation is key to diagnosis and treatment. Cleve Clin J Med 2004; 71 : 489-95. And Mackie SL, Hughes R, Walsh M, Day J, Newton M, Pease C, et al. "An impediment to living life": Why and how should we measure stiffness in polymyalgia rheumatica? PLoS One 2015; 10 : e0126758. As cited in - Milchert M, Brzosko M. Diagnosis of polymyalgia rheumatica usually means a favourable outcome for your patient. Indian Journal Of Medical Research [serial online]. May 2017;145(5):593-600.
- 2 Diamantopoulos AP, Haugeberg G, Lindland A, Myklebust G. The fast-track ultrasound clinic for early diagnosis of giant cell arteritis significantly reduces permanent visual impairment: towards a more effective strategy to improve clinical outcome in giant cell arteritis?. Rheumatology (Oxford). 2016;55(1):66-70.