If a person responds well to nonsurgical treatment for shoulder osteoarthritis, then the arthritic process may be slowed down, pain can be controlled, and surgery may be avoided or at least postponed.
There is a lack of clinical research showing which shoulder arthritis treatments work best for which people. 1 Takamura KM, Chen JB, Petrigliano FA. Nonarthroplasty Options for the Athlete or Active Individual with Shoulder Osteoarthritis. Clin Sports Med. 2018 Oct;37(4):517-526. doi: 10.1016/j.csm.2018.05.003. Review. PubMed PMID: 30201166. , 2 Burbank K.M., Stevenson J.H., Czarnecki G.R., Dorfmon J., "Chronic Shoulder Pain: Part II. Treatment" Am Fam Physician, 2008 Feb 15; 77(4):493-497, http://www.aafp.org, accessed September 2011. This does not mean that treatments are not effective. Rather, it means that a person may need to use a process of trial and error to find the treatment or combination of treatments that work best for him or her.
In This Article:
Home Treatments for Shoulder Osteoarthritis
Common ways to treat shoulder arthritis at home include:
- Activity modification. Cut back on activities that aggravate the shoulder joint and can lead to pain. Intense shoulder activities, such as heavy weight lifting and kayaking, may need to be avoided altogether.
- Periodic rest. A little discomfort in the morning or at the beginning of exercise is normal. Sharp, searing or severe pain is not normal. Moderate to serious shoulder pain is a signal that the joint needs a rest.
- Warm or cold compress. Applying heat, such as using a warming pad, can loosen up a stiff shoulder joint. A cold compress can be applied for 15 or 20 minutes after activity to decrease swelling and pain. Heating or icing a joint may improve symptoms temporarily. They cannot alleviate the underlying causes of shoulder pain.
Other home treatments for shoulder arthritis, such as dietary supplements and electrical stimulation (including transcutaneous electrical nerve stimulation, or TENS) have not been not well studied. Research regarding these treatments typically examines their effects on knee arthritis symptoms rather than shoulder arthritis symptoms.
Physical Therapy
Stretching and strengthening the muscles that support the shoulder joint may reduce shoulder pain and stiffness and increase range of motion. A physical therapist can create an appropriate exercise program, teach it to the patient, and monitor the patient until he or she can be switched to an independent at-home program. Aggressive physical therapy that expands the shoulder’s range of motion may be detrimental. 2 Burbank K.M., Stevenson J.H., Czarnecki G.R., Dorfmon J., "Chronic Shoulder Pain: Part II. Treatment" Am Fam Physician, 2008 Feb 15; 77(4):493-497, http://www.aafp.org, accessed September 2011. A physical therapy program should proceed slowly to maximize benefit.
See Shoulder Exercises for Arthritis
Medications for Shoulder Osteoarthritis
Pain medications can be used to temporarily relieve shoulder arthritis pain.
- Over-the-counter oral pain medication. Analgesics, such as acetaminophen, can reduce pain. Non-steroidal anti-inflammatory drugs (NSAIDs), such as such as aspirin, ibuprofen, and naproxen, can reduce pain as well as the inflammation that contributes to pain. NSAIDs use is associated with gastrointestinal, heart, and kidney problems. 3 Cooper C, Chapurlat R, Al-Daghri N, et al. Safety of Oral Non-Selective Non-Steroidal Anti-Inflammatory Drugs in Osteoarthritis: What Does the Literature Say?. Drugs Aging. 2019;36(Suppl 1):15–24. doi:10.1007/s40266-019-00660-1.
- Prescription oral medication. If shoulder pain does not respond to over-the-counter medications, doctors may recommend prescription-level doses of medications such as naproxen and ibuprofen. Alternatively, they may prescribe other types of medications, such as an NSAID called a COX-2 inhibitor (Celebrex).
- Topical medications. These creams and gels can be applied directly onto the skin over the shoulder. Topical pain relievers come in both prescription and over-the-counter formulas. In general, topical analgesics are less likely than oral medications to cause stomach upset. However, topical medications may not be effective in treating the deep pain of shoulder arthritis.
Doctor and patient should discuss medication in the context of the patient's lifestyle, severity of pain, and medical history. Potential side effects and interactions with other drugs and vitamins/supplements should also be considered.
Injections
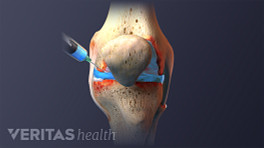
The two types of injections are normally used for treatment of severe pain from shoulder osteoarthritis:
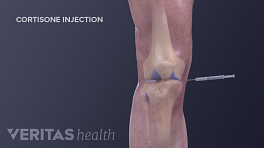
- Steroid injections reduce inflammation and thereby may alleviate shoulder swelling, stiffness, and pain.
- Hyaluronic acid injections provide artificial lubrication for the shoulder joint. Hyaluronic acid mimics the viscous synovial fluid that naturally lubricates joints. Hyaluronic acid injections are a type of treatment called viscosupplementation.
Other types of therapeutic injections, such as platelet-rich plasma (PRP) and stem cell injections, are sometimes offered. While research has been done on these injections in the treatment of knee and hip osteoarthritis, very little research exists regarding their ability to effectively treat shoulder osteoarthritis.
To ensure that an injection is made into the correct location in the shoulder, many experts suggest using ultrasound or fluoroscopy. Fluoroscopy is a radiographic imaging technique that allows doctors to conduct a procedure while watching a real-time X-ray movie. If fluoroscopy is used, contrast fluid is also needed to insure appropriate needle placement and distribution of the injectant (typically a corticosteroid or hyaluronic acid).
If nonsurgical treatment options are tried and the person still has shoulder stiffness and pain, surgery may be recommended.
- 1 Takamura KM, Chen JB, Petrigliano FA. Nonarthroplasty Options for the Athlete or Active Individual with Shoulder Osteoarthritis. Clin Sports Med. 2018 Oct;37(4):517-526. doi: 10.1016/j.csm.2018.05.003. Review. PubMed PMID: 30201166.
- 2 Burbank K.M., Stevenson J.H., Czarnecki G.R., Dorfmon J., "Chronic Shoulder Pain: Part II. Treatment" Am Fam Physician, 2008 Feb 15; 77(4):493-497, http://www.aafp.org, accessed September 2011.
- 3 Cooper C, Chapurlat R, Al-Daghri N, et al. Safety of Oral Non-Selective Non-Steroidal Anti-Inflammatory Drugs in Osteoarthritis: What Does the Literature Say?. Drugs Aging. 2019;36(Suppl 1):15–24. doi:10.1007/s40266-019-00660-1.