There are many similarities in the symptoms of chronic fatigue syndrome, myofascial pain syndrome, and fibromyalgia, increasing the risk of a misdiagnosis.
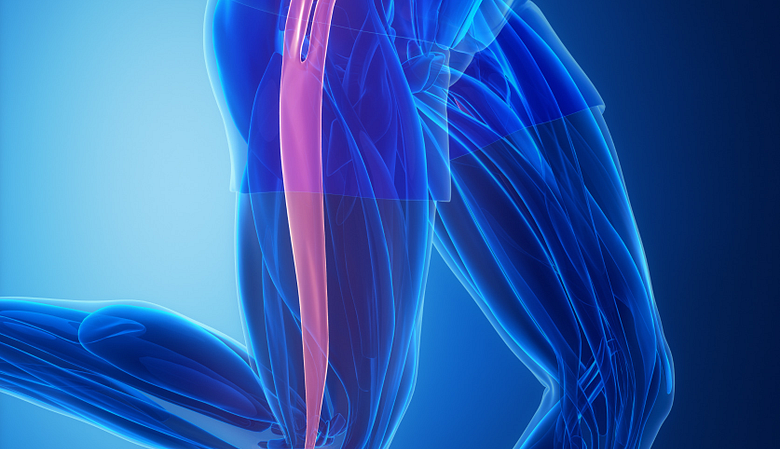
Myofascial pain syndrome occurs when the body's connective tissue is restricted, resulting in pain similar to fibromyalgia.
In This Article:
- Fibromyalgia or Not? 6 Conditions to Know
- Celiac Disease and Low Thyroid vs. Fibromyalgia
- Lyme Disease and Rheumatoid Arthritis (RA) vs. Fibromyalgia
- Chronic Fatigue Syndrome and Myofascial Pain Syndrome vs. Fibromyalgia
Chronic Fatigue Syndrome
Chronic fatigue syndrome and fibromyalgia are so similar that some doctors believe they are the same condition. Others consider the two conditions related. The syndrome is well named; the exhaustion associated with the condition can be debilitating and may last for years.
See Characteristic Symptoms of Fibromyalgia
Chronic fatigue syndrome can develop in children and teens, but is most likely in people between the ages 40 and 60. It is estimated that more than 1 million people in the United States have chronic fatigue syndrome, and the condition is four times more common in women than men. 1 Who's at Risk? Centers for Disease Control and Prevention. Feb. 14, 2013. https://www.cdc.gov/cfs/causes/risk-groups.html
The severe exhaustion, combined with multiple other conditions, forces many people with chronic fatigue syndrome to significantly reduce their activities, and some are unable to continue working.
How it is similar to fibromyalgia. Fatigue, sleep difficulties, stiffness, anxiety, depression, frequent headaches, sensitivity to light, and cognitive issues are common. Other similarities include symptoms of irritable bowel syndrome, symptoms that come and go, and pain in the joints without swelling. There is no single drug that alleviates all the symptoms. The diagnosis is made by ruling out other possible causes.
How it is different from fibromyalgia. Fatigue is the crucial symptom of chronic fatigue syndrome, while pain is the dominant feature with fibromyalgia. The body may also appear to be fighting off an infection, and sore throats may be frequent. Fibromyalgia often appears to stem from a traumatic event, such as a car accident. There is speculation that chronic fatigue syndrome is related to a virus.
Myofascial Pain Syndrome
The weblike connective tissue that covers the muscles throughout the body is known as the fascia, or myofascia. When it is functioning well, the fascia is supple and flexible. If something restricts the movement of the fascia, however, it can cause intense pressure and tension, leading to muscle pain.
Everyone has muscle pain from time to time, but myofascial pain syndrome is more serious. Rather than gradually easing, the pain gets worse and does not go away. Examples of myofascial pain syndrome include acute backache, tension headaches, tennis elbow, and pelvic floor pain, among other conditions.
Watch: Myofascial Pain Syndrome Video
An individual with myofascial pain syndrome may notice knots, or "trigger points," that are painful if pressure is applied. Muscle pain is felt deep inside the muscles. Tightness can be severe enough to restrict movement.
Controversy about the criteria for a diagnosis makes it difficult to know how many people have myofascial pain syndrome. One estimate places the total at about 44 million Americans. 2 Wheeler AH. Myofascial pain disorders: theory to therapy. Drugs. 2004;64(1):45-62. It is not certain what causes myofascial pain syndrome, but hormonal issues, overuse, injuries, and stress are believed to play a role.
How it is different from fibromyalgia: The pain is generally confined to the small knots called trigger points in myofascial syndrome, while pain is widespread and in areas known as tender points in fibromyalgia. Pain does not follow a symmetrical pattern.
How it is similar to fibromyalgia: Muscle pain and tenderness, stiffness, fatigue, sleep problems, headaches, back pain, and depression are common. Trigger point pain may occur in various parts of the body. Lab tests, MRIs, and X-rays usually are not helpful in diagnosing myofascial syndrome. Treatment is multifaceted; no single medication eliminates symptoms.
- 1 Who's at Risk? Centers for Disease Control and Prevention. Feb. 14, 2013. https://www.cdc.gov/cfs/causes/risk-groups.html
- 2 Wheeler AH. Myofascial pain disorders: theory to therapy. Drugs. 2004;64(1):45-62.