Subscribe to our newsletter and get your FREE guide,
Natural Back Pain Relief: 16 Choices for Lasting Comfort.
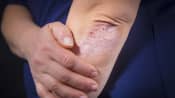
What Is Psoriatic Arthritis?
Peer-Reviewed Article
Psoriatic arthritis is a medical condition including skin psoriasis, joint pain, and swelling. Subtypes include asymmetric, symmetric, distal, mutilans, and axial.