Arthritis is often the underlying cause of knee pain in absence of an injury. This article describes 6 types of arthritis that can affect the knee.
1. Osteoarthritis
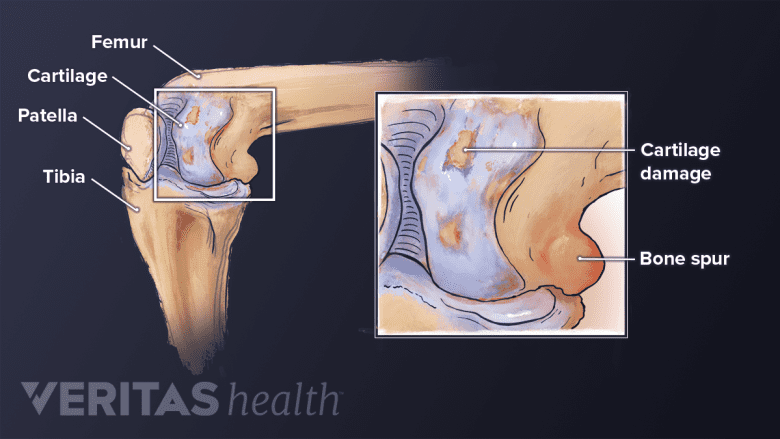
Osteoarthritis is caused by cartilage degeneration and bony protrusions called osteophytes.
The most common type of arthritis affecting the knee is osteoarthritis. Osteoarthritis occurs when a joint’s articular cartilage breaks down. In the knee, articular cartilage covers the top of the tibia (shin bone), bottom of the femur (thigh bone), and back of the patella (knee cap).
See What Is Knee Osteoarthritis?
Not everyone with knee osteoarthritis will get knee pain. Pain may occur if the loss of healthy cartilage:
- Causes the bones of the joint to rub against one another.
- Compromises the joint’s biomechanics in some other way.
Watch Knee Osteoarthritis Video
In the early stages of knee osteoarthritis, pain may be felt when doing specific activities, such as jogging. As osteoarthritis progresses, pain may be felt during daily activities.
See Knee Osteoarthritis Symptoms
Post-traumatic knee arthritis
Post-traumatic arthritis is a type of osteoarthritis. It develops after a meniscus tear, ligament injury, or other trauma. The injury may heal but wear-and-tear on the articular cartilage can accelerate. Post-traumatic arthritis may not become symptomatic until years after the injury.
Watch Knee Meniscus Tear Video
2. Rheumatoid Arthritis
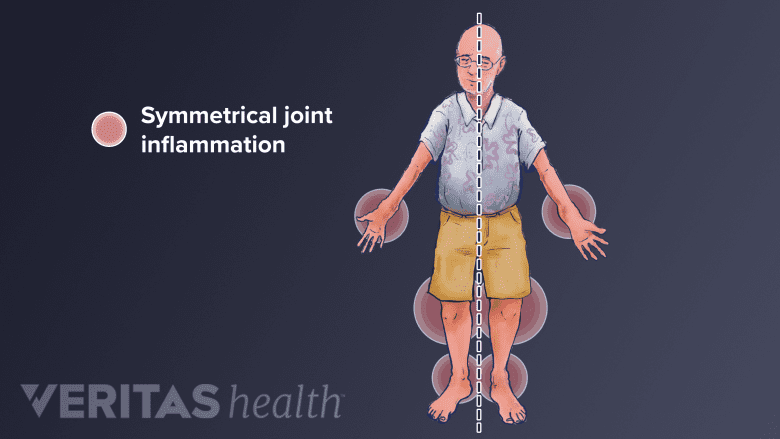
Rheumatoid arthritis is an autoimmune disease that targets the membrane surrounding joints.
Knee pain can be caused by an autoimmune disease called rheumatoid arthritis (RA). RA causes joint inflammation that can make the knee feel swollen, stiff, warm, and painful. Over time, untreated RA can cause permanent knee joint damage.
See What Is Rheumatoid Arthritis (RA)?
Rheumatoid arthritis often affects joints symmetrically, so if one knee is affected the other is also likely to be affected. Symptoms are also common in the hands and wrists. Episodes of RA may come and go and can be accompanied by other symptoms, such as fatigue.
See Rheumatoid Arthritis (RA) Symptoms
3. Psoriatic Arthritis

Psoriatic arthritis is an autoimmune disease associated with psoriasis, a skin condition.
Like rheumatoid arthritis, psoriatic arthritis is an autoimmune disease. When the knee is affected by psoriatic arthritis, the knee may feel painful, stiff, swollen, and tender. Other joints are often affected, particularly joints in the fingers and toes. Other common symptoms include fatigue and eye pain.
See What Is Psoriatic Arthritis?
Psoriasis is a skin condition. While estimates vary, recent research suggests about 20% of people with psoriasis also have psoriatic arthritis.1Alinaghi F, Calov M, Kristensen LE, et al. Prevalence of psoriatic arthritis in patients with psoriasis: A systematic review and meta-analysis of observational and clinical studies. J Am Acad Dermatol. 2018; Many people have psoriasis for years before experiencing joint pain associated with psoriatic arthritis.
See Psoriatic Arthritis Causes
4. Gout
Gout is an inflammatory arthritis that can cause a build-up of uric acid crystals (monosodium urate crystals) in the knee joint. These needle-like, microscopic crystals collect in the soft tissue of the knee joint, causing pain that can be excruciating, as well as swelling, redness, and warmth.
See All About Gout - Symptoms, Diagnosis, Treatment
About half of all gout cases affect the big toe joint (metatarsophalangeal joint), but other cases affect the knee or another joint.
5. Pseudogout: Calcium Pyrophosphate Deposition (CPPD)
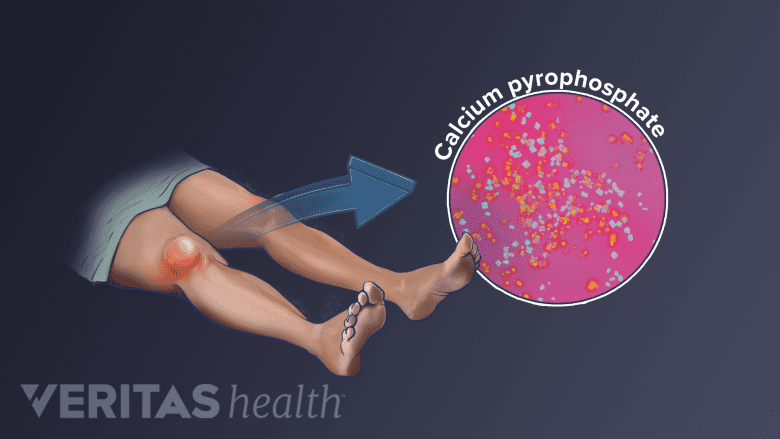
Pseudogout is type of arthritis caused by the buildup of calcium pyrophosphate crystals in joints.
Like gout, pseudogout is caused by a build-up of microscopic crystals in a joint and can lead to sudden, severe knee pain, swelling, warmth, and redness. Pseudogout is less common than gout but more likely to affect the knee joint.
See All About Pseudogout - Symptoms, Diagnosis, Treatment
The microscopic crystals that cause pseudogout are called calcium pyrophosphate crystals. Doctors often refer to pseudogout as calcium pyrophosphate deposition (CPPD).
6. Reactive Arthritis
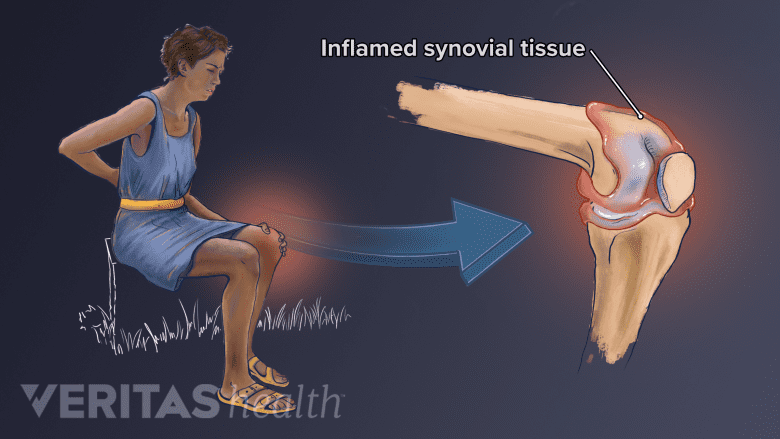
Reactive arthritis causes inflammatory joint pain, often in the knees, fingers, or low back.
Reactive arthritis commonly affects the knee, though it can affect any joint. Arthritis inflammation can make a knee achy, swollen, and/or red.
See Reactive Arthritis Symptoms
Reactive arthritis develops as a reaction to an infection, such as a stomach bug or a sexually transmitted disease (STD). Days, weeks, or even months after the infection has resolved, a person may develop pain in one or more joints, inflamed eyes, and/or other symptoms.
See Infections that Can Cause Reactive Arthritis
The above conditions are common causes of arthritic knee pain. There are more than 100 types of arthritis that may include knee symptoms. People with chronic knee pain are advised to consult with their doctors for accurate diagnoses.
- 1 Alinaghi F, Calov M, Kristensen LE, et al. Prevalence of psoriatic arthritis in patients with psoriasis: A systematic review and meta-analysis of observational and clinical studies. J Am Acad Dermatol. 2018;

