Simple tasks such as gripping a toothbrush or turning a doorknob can be difficult when rheumatoid arthritis inflammation affects the hands. The joints in the fingers and wrists may feel too painful, stiff, and weak to function normally.
This article reviews how RA affects hand function, the joints most typically affected, and how RA inflammation develops in the joint tissues of the hands, potentially causing conditions such as tenosynovitis and carpal tunnel syndrome. The hallmark signs and symptoms of hand RA, potential hand deformities, and treatment options are also discussed.
In This Article:
- Hand Pain and Rheumatoid Arthritis
- Hand Rheumatoid Arthritis Signs and Symptoms
- Treatments for Rheumatoid Arthritis in Hands
How Rheumatoid Arthritis Affects Hand Function
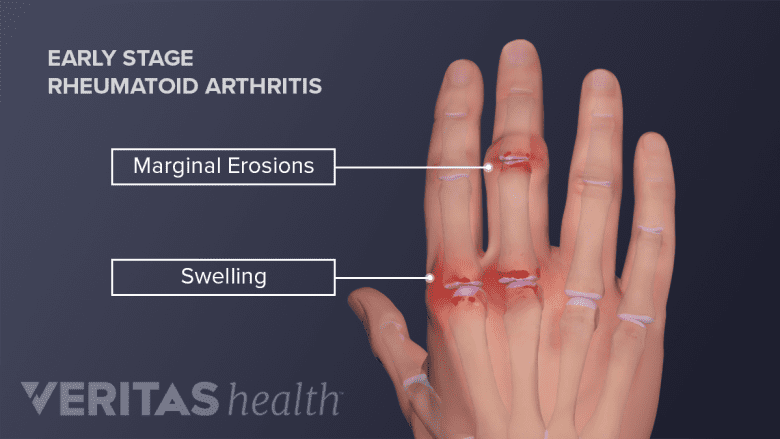
Swelling and bone erosion at the margins of the joint can be the first signs of RA.
Rheumatoid arthritis (RA) is a chronic systemic autoimmune disease. RA symptoms appear in the hand when the immune system mistakenly attacks joint tissues in the fingers, thumb, and/or wrist.
Researchers have found:
- Hand dexterity, grip strength, and the ability to pinch objects between the thumb and fingers are likely to be affected by RA.,
- Grip strength may be even weaker when RA inflammation levels are high.,
- Problems with hand function tend to be the result of RA joint damage.
Joint damage can weaken tendons and cause joints to become malaligned or deformed. A significant amount of joint damage happens early on in the disease process, which is why early diagnosis and treatment are important.
See Blood Tests to Help Diagnose Rheumatoid Arthritis (RA)
Hand Joints Most Affected By Rheumatoid Arthritis
There are 27 joints in a hand. The joints most likely to show signs of RA are:
- The metacarpophalangeal (MCP) joints, or large knuckles, where the fingers and thumb meet the hand
- The proximal interphalangeal (PIP) joints, or middle knuckles
- The joints of the wrist that connect the wrist’s eight carpal bones with each other and the bones of the forearm (the radius and ulna), including the carpometacarpal joint, midcarpal joint, radiocarpal joint, and intercarpal joints
The distal interphalangeal (DIP) joints, the joints closest to the tips of the fingers and thumb, are less likely to be affected by rheumatoid arthritis. When DIP joints are affected, it is typically only after symptoms appear in the MCP or PIP joints. It is more common for DIP joints to be affected by osteoarthritis than by RA.
See Recognizing Osteoarthritis in the Hand
Hand joints are synovial joints
The small joints of the hands are an example of synovial joints. (Most flexible joints in the body, including the knees, hips, and shoulders, are also synovial joints.) Rheumatoid arthritis attacks synovial joints.
- Each synovial joint is encapsulated in a pliable membrane, called a synovial membrane or synovium. When the joint is healthy, this membrane is very thin—just one or two cells thick.
- The joint capsule contains synovial fluid. This fluid is produced by the membrane. It is thin, clear, and viscous, and it normally nourishes and lubricates the joint, enabling movement.
Synovial joints in the hand are quite small and normally contain just a tiny amount of synovial fluid.
How Rheumatoid Arthritis Develops
When rheumatoid arthritis occurs, the immune system attacks a synovial joint’s delicate membrane. The affected finger, thumb, and/or wrist joints can become inflamed, swollen, and painful.
The disease process involves these 5 steps:
- White blood cells invade. The immune system sends white blood cells, called leukocytes, to invade one or more hand joints.
- Inflammation is triggered. The white blood cells trigger inflammation in the hand joints’ synovium. When synovium is inflamed it is called synovitis.
- Pannus forms. The inflamed synovial tissue may continue to react to the white blood cell invasion by adding layers of new synovial cells at a very rapid pace. This new, abnormal tissue is called pannus.
- Cartilage and bone are damaged. The rheumatoid pannus tissue squeezes into the joint space between bones and releases proteins that degrade the hand joints’ articular cartilage, ligaments, and bone. The parts of the bone that are not protected by cartilage are typically the first sites of damage; this is referred to as marginal erosion.
- Excess fluid is produced. In addition to releasing damaging proteins, the pannus may create excess fluid that contributes to wrist and knuckle swelling.
Changes can also occur in the hand’s tendons.
Tenosynovitis in the Hands
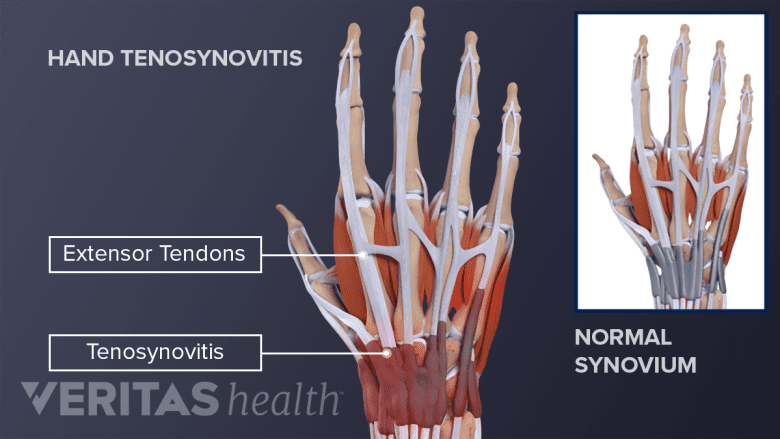
Inflammation of the flexor tendon or tendon sheath in the hand can lead to trigger finger and may indicate rheumatoid arthritis.
In addition to encapsulating joints, synovial tissue also surrounds most tendons. Tendons connect muscles to bones. Rheumatoid arthritis can cause a tendon’s synovial sheath to become inflamed, a condition called tenosynovitis. The inflammation is not always painful but can lead to tendon damage.
In the hand, flexor tendons allow a person to bend their fingers. When a finger’s flexor tendon is inflamed it can cause the middle knuckle (PIP joint) to get stuck in a bent position. This condition is called trigger finger.
At least one study suggests that tenosynovitis of flexor tendons is a strong predictor of rheumatoid arthritis.
How RA Causes Hand Pain
Changes to the hand joint can be seen and felt. Inflammation can cause significant pain, swelling, and stiffness. In addition, joint degeneration and abnormalities can put excess strain on already damaged tendons and other tissues, leading to pain.
When Rheumatoid Arthritis in the Hand Is Serious
Experts estimate 90% of people who have RA have symptoms in at least one hand joint., While prompt and aggressive treatment can typically prevent the worst outcomes, RA in the hand can be a serious cause for concern if:
- Damage to joint tissues causes bones to become malaligned. This malalignment can result in hand deformities and prevent the hand from functioning normally.
- It prevents a person from being able to care for themselves, particularly if they live alone.
- It leads to severe carpal tunnel syndrome. Advanced carpal tunnel causes numbness and/or tingling and weakness in the thumb and associated fingers, and can result in permanent nerve damage if left untreated.
In any of these cases, consultation with a medical professional is advised.