Joint inflammation and pain can be caused by a bacterial, viral, or fungal infection, and sometimes these symptoms are initially mistaken for rheumatoid arthritis (RA). People who have joint pain and a fever that they suspect is caused by an infection are advised to seek medical attention.
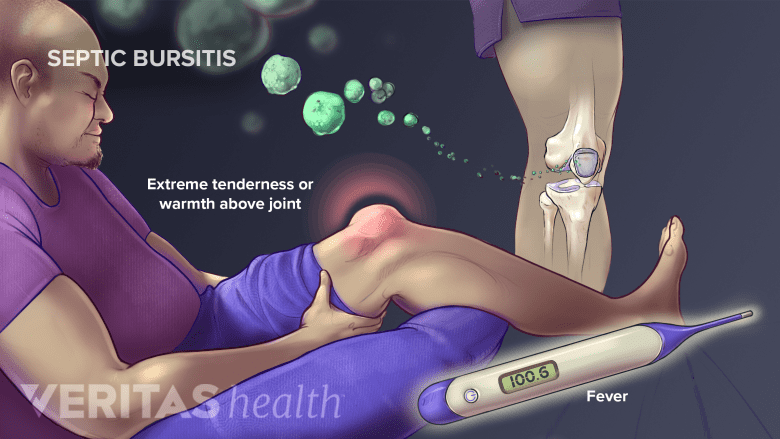
Septic bursitis may create some symptoms similar to rheumatoid arthritis. It requires immediate medical attention.
In This Article:
- Are My Painful Joints Caused By Rheumatoid Arthritis (RA) or Something Else?
- Is My Joint Pain Rheumatoid Arthritis (RA) or Spondyloarthropathy?
- Is My Joint Pain Caused By Rheumatoid Arthritis (RA) or a Crystal Arthritis?
- Is My Joint Pain Caused by Rheumatoid Arthritis (RA) or an Infection?
- Is My Joint Pain Caused by Rheumatoid Arthritis (RA) or Another Autoimmune Disorder?
- Rheumatoid Arthritis Overview Video
Viral Arthritis vs. Rheumatoid Arthritis
Experts estimate about 1% of arthritis cases to be viral arthritis.1Marks M, Marks JL. Viral arthritis. Abstract only. Clin Med (Lond). 2016 Apr;16(2):129-34. doi: 10.7861/clinmedicine.16-2-129. PubMed PMID: 27037381. In these cases, a viral infection leads to joint pain and swelling. For example, parvovirus B19, known for causing fifth disease (erythema infectiosum), sometimes causes swollen, painful joints and anemia. Other examples of viruses that can cause viral arthritis include enterovirus, rubella, HIV, and hepatitis B and C.
How is it similar to RA? Viral arthritis results in inflamed joints that are swollen, tender, red, and warm to the touch.
How is it different? There is no specific blood test for RA, but a blood test can usually show whether or not a person has or had a particular virus. The joint symptoms will typically go away once the viral infection is either treated or resolves on its own, though in some cases arthritis symptoms become chronic.
See Rheumatoid Arthritis (RA) Symptoms
Lyme Disease vs. Rheumatoid Arthritis
Lyme disease is a bacterial infection spread to humans by infected deer ticks and western blacklegged ticks. Some people do not know they have been bitten, making diagnosis challenging. A doctor may consider a Lyme disease diagnosis if the patient experienced a bulls-eye shaped rash or has been in area where deer ticks and Lyme disease thrive, such as forested areas of the East Coast and upper Midwest.
See Lyme Disease and Rheumatoid Arthritis (RA) vs. Fibromyalgia
How is it similar to RA? Lyme disease can cause joint pain, fatigue, and a fever.
See Risk Factors for Rheumatoid Arthritis (RA)
How is it different? People with Lyme disease often report headaches and/or stiff necks. Lymph nodes may become swollen and muscles may ache. A fever may be accompanied by the chills.
A blood test can show the presence of Lyme disease, but it cannot be done until 2 or 3 weeks after the tick bite, and results are not always accurate. (A more precise blood test is available, but accurate results require the test be done several weeks after exposure.)
Experts recommend treating suspected Lyme disease with antibiotics as soon as possible, often before lab tests can confirm a diagnosis.
Septic Arthritis vs. Rheumatoid Arthritis
Sometimes an infection in a joint can cause severe inflammation, pain, and swelling. Most septic arthritis is caused by a bacterium called Staphylococcus aureus (sometimes called a “staph infection”).
Septic arthritis occurs when a bacteria, virus, or fungus elsewhere in the body travels through the blood stream and invades the joint. It can also occur when an infectious organism reaches the joint through a break in the skin (e.g. a cut or eczema rash), though this is less common.
See Psoriatic Arthritis Symptoms
How is it similar to RA? Infectious arthritis results in an inflamed joint that is swollen, tender, red, and warm to the touch. Often just one joint is affected. People with infectious arthritis may also have a fever and/or feel unwell.
How is it different? Joint symptoms usually appear suddenly and are often severe, so that the person cannot use the affected joint. Lab tests can confirm whether or not a joint is infected.
People who have weakened immune systems, including people who take RA medications, are at an increased risk for septic arthritis.
The Differences Between Infectious and Reactive Arthritis
Reactive arthritis occurs when the immune system overreacts to an infection, causing it to attack the joints. The organism that caused the original infection—usually a type of bacteria—is not causing the joint symptoms. In fact, the person may be completely recovered from his or her illness and no longer have symptoms from the original infection.
See Reactive Arthritis Survival Guide
In contrast, a person with infectious arthritis has an existing infection and the infectious organism (e.g. bacterium) may be present in the affected joint capsule.
See Infections that Can Cause Reactive Arthritis
Some experts consider reactive arthritis to be a type of infectious arthritis.2Infectious Arthritis. Medline Plus. NIH National Library of Medicine. https://www.nlm.nih.gov/medlineplus/infectiousarthritis.html Last Reviewed July 2014. Accessed April 5, 2016.
- 1 Marks M, Marks JL. Viral arthritis. Abstract only. Clin Med (Lond). 2016 Apr;16(2):129-34. doi: 10.7861/clinmedicine.16-2-129. PubMed PMID: 27037381.
- 2 Infectious Arthritis. Medline Plus. NIH National Library of Medicine. https://www.nlm.nih.gov/medlineplus/infectiousarthritis.html Last Reviewed July 2014. Accessed April 5, 2016.

