A lime- or grapefruit-sized lump at the front of the knee may be a sign of prepatellar bursitis. Prepatellar bursitis occurs when the bursa at the front of the knee becomes inflamed and fills with excess fluid.
An adult body contains about 140 bursae.1Azar FM, Beaty JH, Canale TS, eds. Campbell’s Operative Othopaedics, 13th ed., vol 1, page 482. Philadelphia PA: Elsevier; 2017. The prepatellar bursa is located at the front of the knee, in between the skin and the patella bone (kneecap). It is one of the bursae most likely to develop bursitis.
In This Article:
What Causes Bursitis in the Knee?
To understand what causes knee bursitis, it is helpful to know more about the prepatellar bursa and bursae in general:
- A bursa is a thin, slippery, fluid-filled sac that serves as both a cushion and a lubricant between kneecap and skin.
- The prepatellar bursa is normally just 0.1 inch thick—about the thickness of 2 quarters stacked on top of each other—and 1.5 inches in diameter.2Aguiar RO, Viegas FC, Fernandez RY, Trudell D, Haghighi P, Resnick D. The prepatellar bursa: cadaveric investigation of regional anatomy with MRI after sonographically guided bursography. AJR Am J Roentgenol. 2007 Apr;188(4):W355-8. doi: 10.2214/AJR.05.1466. PubMed PMID: 17377004.
- When inflamed, a bursa’s normally thin lining thickens and produces excess fluid. The excess fluid collects in the bursa sac, causing it to swell.
- When the prepatellar bursa is inflamed, it fills with fluid, causing the front of the knee to look swollen.
There are many reasons a prepatellar bursa may become inflamed, such as repeated irritation, an injury, or an underlying inflammatory condition. Repeated irritation from kneeling is the most common reason.
See Causes of Knee Bursitis (Prepatellar Bursitis)
Housemaid’s knee and other nicknames
Prepatellar bursitis has been called housemaid’s knee, carpet layer’s knee, coal miner’s knee, and carpenter's knee. These nicknames arose because people whose jobs require frequent kneeling are prone to knee bursitis.
Who Gets Knee Bursitis?
While anyone can get prepatellar bursitis, experts estimate about 80% of cases occur in men. Men aged 40 to 60 years are most likely to be affected.3Baumbach SF, Lobo CM, Badyine I, Mutschler W, Kanz KG. Prepatellar and olecranon bursitis: literature review and development of a treatment algorithm. Arch Orthop Trauma Surg. 2014 Mar;134(3):359-70. doi: 10.1007/s00402-013-1882-7. Epub 2013 Dec 5. PMID: 24305696.
How Long Does Knee Bursitis Last?
With rest and home treatment, the swelling and other symptoms caused by knee bursitis may go away in a couple of weeks. Medical treatment may be necessary if symptoms persist longer than 2 or 3 weeks after beginning rest and home treatment.
Knee bursitis that does not go away or comes and goes repeatedly is considered chronic bursitis. When knee bursitis is chronic it is more challenging to treat.
What Does Knee Bursitis Feel Like?
When pressed, the lump at the front of the knee may feel like a water balloon. The knee may also feel tender, stiff, and painful.
Interestingly, prepatellar bursitis is not always painful.4Williams CH, Sternard BT. Bursitis. [Updated 2020 Aug 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513340/ Little or no pain is especially likely when prepatellar bursitis has become chronic.5Khodaee M. Common Superficial Bursitis. Am Fam Physician. 2017 Feb 15;95(4):224-231. PMID: 28290630.
See Prepatellar Bursitis Symptoms
Knee pain, along with skin that is warm to the touch, may be a sign of infection. An infected bursa (septic bursitis) is a serious condition and requires immediate medical attention.
Can Knee Bursitis Be Serious?
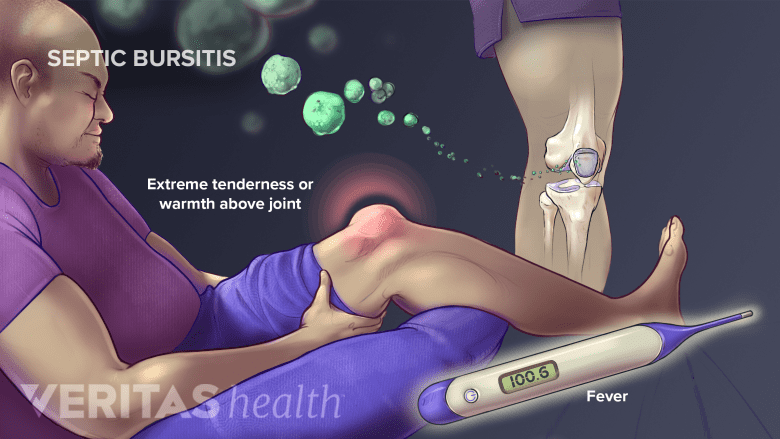
Septic knee bursitis occurs due to infection of the bursa and requires immediate medical attention.
Experts estimate about 1/3 of prepatellar bursitis cases may be caused by an infection.3Baumbach SF, Lobo CM, Badyine I, Mutschler W, Kanz KG. Prepatellar and olecranon bursitis: literature review and development of a treatment algorithm. Arch Orthop Trauma Surg. 2014 Mar;134(3):359-70. doi: 10.1007/s00402-013-1882-7. Epub 2013 Dec 5. PMID: 24305696. When a bursa is infected the bursa sac fills with puss. This condition is called septic bursitis, and requires urgent treatment.
Septic prepatellar bursitis
A person with septic prepatellar bursitis may notice the skin over the knee:
- Appears red
- Is noticeably warmer than other areas
- Looks patchy or has a rash, bumps, or sores (indicating a skin infection)
Septic bursitis can also cause body-wide symptoms, such as:
- Fever
- Fatigue
- A general feeling of being sick
Septic bursitis is common in the prepatellar bursa because it lies just below the skin. Bursae that lie just below the skin are called superficial bursae. Bacteria and other microorganisms typically enter a superficial bursa through a scrape or cut. Less often, microorganisms enter a bursa during an aspiration, a procedure to remove fluid from the bursa.5Khodaee M. Common Superficial Bursitis. Am Fam Physician. 2017 Feb 15;95(4):224-231. PMID: 28290630.
It is possible for an infection to occur without an obvious entry point on the skin.
Seek immediate treatment
Without treatment, the infectious microbes (typically bacteria) in the bursa may spread to other areas of the leg or the bloodstream. An infection of the bloodstream is rare5Khodaee M. Common Superficial Bursitis. Am Fam Physician. 2017 Feb 15;95(4):224-231. PMID: 28290630. but can be life-threatening.
To prevent the spread of infection, experts strongly advise treating septic bursitis immediately. Oral antibiotics can treat most cases of septic bursitis.
Are There Other Types of Knee Bursae?
There are up to 30 bursae in the knee.6Paulsen F, Waschke J. Sobotta Clinical Atlas of Human Anatomy. Elsevier. 2019. While bursitis is most likely to develop in the prepatellar bursa, it occasionally develops in others. A few examples of other types of knee bursitis include:
Pes anserine bursitis
Symptoms of pes anserine bursitis typically include pain and swelling on the inside (medial side) of the knee, 2 or 3 inches below the actual knee joint. The pes anserine bursa reduces friction between the shin’s tibia bone and the tendons of the hamstring muscles.
Watch Pes Anserine Bursitis Video
Iliotibial bursitis
Symptoms of iliotibial bursitis include pain and swelling at the outside (lateral side) of the knee. The iliotibial bursa reduces friction between the shin’s tibia bone and the iliotibial band (IT band), a thick, fibrous tissue that extends from the outer hip to just below the knee.
Iliotibial bursitis is associated with a tight IT band.7Chatra PS. Bursae around the knee joints. Indian J Radiol Imaging. 2012;22(1):27-30. doi: 10.4103/0971-3026.95400
Read more about Iliotibial Band Syndrome on Sports-health.com
Infrapatellar bursitis
Another bursa, called the infrapatellar bursa, is located just below the prepatellar bursa. It lies between the skin and the knobby top of the shinbone (tibia). It is rare for bursitis to occur in the infrapatellar bursa.5Khodaee M. Common Superficial Bursitis. Am Fam Physician. 2017 Feb 15;95(4):224-231. PMID: 28290630.
Septic bursitis is not common in the pes anserine and iliotibial bursae, which lie deep below the skin.
While this article focuses on prepatellar bursitis, many of the concepts presented also apply to other types of bursitis.
What Other Conditions Cause Knee Swelling?
Prepatellar bursitis is typically easy to diagnose because it causes significant swelling at the front of the knee. Other types of arthritis that commonly cause knee swelling include:
- Gout
- Pseudogout
- Osteoarthritis
- Rheumatoid arthritis
These conditions tend to affect knee function more than knee bursitis. For example, putting weight on a gouty knee may be excruciatingly painful.
For a full list and description of conditions that cause knee swelling, read What Causes a Swollen Knee (Water on the Knee)?
What Type of Doctor Treats Knee Bursitis?
Many doctors are qualified to diagnose and make treatment recommendations for knee bursitis. Examples include:
- Primary care providers, such as family medicine doctors and internists
- Doctors who specialize in sports medicine, such as physiatrists
- Orthopedists
- Rheumatologists
A doctor may refer a patient to another specialist depending on the patient’s unique health circumstances.
- 1 Azar FM, Beaty JH, Canale TS, eds. Campbell’s Operative Othopaedics, 13th ed., vol 1, page 482. Philadelphia PA: Elsevier; 2017.
- 2 Aguiar RO, Viegas FC, Fernandez RY, Trudell D, Haghighi P, Resnick D. The prepatellar bursa: cadaveric investigation of regional anatomy with MRI after sonographically guided bursography. AJR Am J Roentgenol. 2007 Apr;188(4):W355-8. doi: 10.2214/AJR.05.1466. PubMed PMID: 17377004.
- 3 Baumbach SF, Lobo CM, Badyine I, Mutschler W, Kanz KG. Prepatellar and olecranon bursitis: literature review and development of a treatment algorithm. Arch Orthop Trauma Surg. 2014 Mar;134(3):359-70. doi: 10.1007/s00402-013-1882-7. Epub 2013 Dec 5. PMID: 24305696.
- 4 Williams CH, Sternard BT. Bursitis. [Updated 2020 Aug 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513340/
- 5 Khodaee M. Common Superficial Bursitis. Am Fam Physician. 2017 Feb 15;95(4):224-231. PMID: 28290630.
- 6 Paulsen F, Waschke J. Sobotta Clinical Atlas of Human Anatomy. Elsevier. 2019.
- 7 Chatra PS. Bursae around the knee joints. Indian J Radiol Imaging. 2012;22(1):27-30. doi: 10.4103/0971-3026.95400

