Doctors sometimes refer to knee swelling as “knee effusion.” Others may refer to it as "water on the knee." Knee swelling can result from an injury, chronic overuse, or a disease.
Swelling in a knee joint may limit knee flexibility and function. For example, a person may find it difficult to fully bend or completely straighten a swollen knee, and the joint may naturally bend 15° to 25° while the leg is at rest. 1 Johnson MW. Acute knee effusions: a systematic approach to diagnosis. Am Fam Physician. 2000 Apr 15;61(8):2391-400. Review. PubMed PMID: 10794580. The swollen knee may also be painful, red, and/or difficult to put weight on.
Depending on the underlying condition, a swollen knee may be treated at home using the R.I.C.E. formula (rest, ice, compression, and elevation) or may require medical treatment. A doctor can make an accurate diagnosis.
In This Article:
- What Causes a Swollen Knee (Water on the Knee)?
- More Causes of a Swollen Knee (Water on the Knee)
12 Potential Causes of Knee Swelling

Knee swelling, if not a septic infection, may often be approached with home treatments.
Whether water on the knee is mildly annoying or painfully debilitating, a person will want to identify the likely cause and treat the symptoms to help reduce the likelihood of future problems. Chronic or long-standing swelling may lead to joint tissue damage, cartilage degradation, and bone softening, therefore treatment is usually recommended.
This article describes 12 conditions that frequently cause knee swelling, also called water on the knee.
1. Injury to the knee
Trauma to the knee's bones, ligaments, tendons, bursae, meniscus, or articular cartilage can cause pain and swelling. Serious injury can cause blood to flood into the knee joint, leading to significant swelling, warmth, stiffness, and bruising. This condition is called hemarthrosis and warrants urgent medical care.
A patient should also seek medical attention if knee pain is severe, if the affected leg cannot bear weight, or if there is suspicion of a broken bone.
2. Knee osteoarthritis

Overuse and degeneration of the cartilage in the knee joint may cause water on the knee.
Degeneration of the cartilage of the knee joint can result in an overproduction of joint fluid, causing the knee to swell. A swollen knee due to knee osteoarthritis is typically accompanied by pain.
In fact, evidence suggests people who have severe knee pain from osteoarthritis are more likely to experience knee swelling. One study 2 Kraus VB, Stabler TV, Kong SY, Varju G, McDaniel G. Measurement of synovial fluid volume using urea. Osteoarthritis Cartilage. 2007;15(10):1217-1220. doi:10.1016/j.joca.2007.03.017 found that:
- People who reported mild to moderate osteoarthritic knee pain had an average of 7.0 ml of joint fluid in the affected knee—which is about the same as a healthy knee. 3 Heilmann HH, Lindenhayn K, Walther HU. Das Synovia-Volumen gesunder und arthrotischer menschlicher Kniegelenke [Synovial volume of healthy and arthrotic human knee joints]. Z Orthop Ihre Grenzgeb. 1996;134(2):144-148. doi:10.1055/s-2008-1039786
- People who reported severe osteoarthritic knee pain had an average of more than 20 ml (about 4 teaspoons) of fluid in the affected knee.
Knee swelling caused by osteoarthritis is typically mild to moderate. When swelling is severe, another problem may be the cause.
There are numerous home treatments for knee osteoarthritis. A doctor can also prescribe medical treatments, such as physical therapy, and perform therapeutic injections.
3. Bursitis (non-septic or septic)
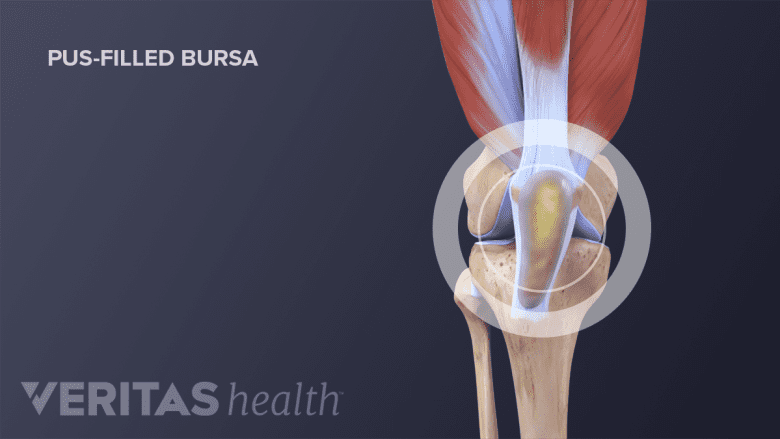
When a knee bursa is filled with pus, the knee may appear swollen and red, and may feel warm and painful.
Throughout the body are tiny, thin, fluid-filled sacs called bursae. These slippery cushions reduce friction between bone and surrounding soft tissue, such as skin and muscle. The knee has 11 bursae, and 2 of them are especially susceptible to bursitis.
When a bursa becomes inflamed it is called bursitis. An inflamed knee bursa can fill with excess fluid, causing swelling, or water on the knee. The swollen knee may feel "squishy," like a water balloon. It may or may not be tender and painful. The most common types of knee bursitis are prepatellar bursitis and pes anserine bursitis.
While most cases of bursitis can be treated with at-home and non-urgent medical care, septic bursitis can be life-threatening. This condition occurs when a bursa has been infected with a microorganism. The bursa can become inflamed and fill with pus. The swollen knee may appear red and feel hot, and the person may have a fever and/or feel unwell.
People should seek medical attention immediately if they think their symptoms may be caused by septic bursitis.
4. Gout
A painful accumulation of microscopic uric acid crystals in the joint defines a gout attack. This swelling often occurs at night, while lying in bed. It typically occurs rapidly and is accompanied by sudden, excruciating pain, redness, and warmth.
While gout is most likely to affect the big toe, it also commonly affects the knee as well as the heel, ankle, and foot instep. 4 Sidari A, Hill E. Diagnosis and Treatment of Gout and Pseudogout for Everyday Practice. Prim Care. 2018;45(2):213-236. doi:10.1016/j.pop.2018.02.004 Gout typically affects just one joint at a time. First-time gout attacks typically occur in men in their 30s, 40s, and 50s.
While an episode of gout usually resolves on its own, medication and medical treatment can help relieve the pain and other symptoms. Many people can lower their chances of future gout attacks—and the joint damage they can cause—by making dietary changes. Oral medications may also be prescribed.
See Gout Treatment
5. Pseudogout
Less common but similar to gout, pseudogout is also caused by an accumulation of microscopic crystals in a joint. Calcium pyrophosphate crystals can accumulate in a knee joint and cause sudden, severe pain, and swelling. The skin over the affected joint may appear discolored.
Pseudogout occurs most frequently in the knee and can also affect the shoulder, elbow, ankle, wrist, large knuckles, hip, or spine. It may affect more than one joint at a time and may be mistaken for rheumatoid arthritis or osteoarthritis. 5 Ivory D, Velázquez CR. The forgotten crystal arthritis: calcium pyrophosphate deposition. Mo Med. 2012;109(1):64-68. Doctors often refer to pseudogout as calcium pyrophosphate deposition (CPPD) or acute calcium pyrophosphate crystal arthritis (acute CPP crystal arthritis).
Old age is the most significant risk factor for pseudogout. An episode of pseudogout usually goes away in a couple of weeks. 5 Ivory D, Velázquez CR. The forgotten crystal arthritis: calcium pyrophosphate deposition. Mo Med. 2012;109(1):64-68. Medication and medical treatment can help relieve the pain.
6. Rheumatoid arthritis
An autoimmune disease that affects the delicate lining of the joints, rheumatoid arthritis can cause knee swelling, stiffness, pain, tenderness, and redness. The knee may feel “spongy” when pressed.
Although the knees can exhibit symptoms, the hands, wrists, and feet are more often affected by rheumatoid arthritis. RA tends to affect joints symmetrically, so if the right knee is affected the left knee may also be affected.
In addition to joint pain and swelling, rheumatoid arthritis can cause other symptoms, such as fatigue, low-grade fever, and a general feeling of being unwell. Prompt diagnosis and treatment of rheumatoid arthritis can help minimize long-term joint damage.
See Rheumatoid Arthritis (RA) Symptoms
Read on to learn more causes of a swollen knee.
- 1 Johnson MW. Acute knee effusions: a systematic approach to diagnosis. Am Fam Physician. 2000 Apr 15;61(8):2391-400. Review. PubMed PMID: 10794580.
- 2 Kraus VB, Stabler TV, Kong SY, Varju G, McDaniel G. Measurement of synovial fluid volume using urea. Osteoarthritis Cartilage. 2007;15(10):1217-1220. doi:10.1016/j.joca.2007.03.017
- 3 Heilmann HH, Lindenhayn K, Walther HU. Das Synovia-Volumen gesunder und arthrotischer menschlicher Kniegelenke [Synovial volume of healthy and arthrotic human knee joints]. Z Orthop Ihre Grenzgeb. 1996;134(2):144-148. doi:10.1055/s-2008-1039786
- 4 Sidari A, Hill E. Diagnosis and Treatment of Gout and Pseudogout for Everyday Practice. Prim Care. 2018;45(2):213-236. doi:10.1016/j.pop.2018.02.004
- 5 Ivory D, Velázquez CR. The forgotten crystal arthritis: calcium pyrophosphate deposition. Mo Med. 2012;109(1):64-68.

