The pain and stiffness caused by shoulder osteoarthritis can affect arm movement. It can be painful and difficult to hit a golf ball, lift a dish from a kitchen cupboard, or even brush teeth. Even moderate shoulder osteoarthritis can cause chronic dull pain or intermittent flare-ups of intense pain that interrupt sleep.

Shoulder osteoarthritis involves degenerative changes to the cartilage and other structures in the glenohumeral joint.
Shoulder osteoarthritis may be referred to as glenohumeral osteoarthritis or simply shoulder arthritis. Osteoarthritis is the most common form of arthritis to affect the shoulder. Inflammatory forms of arthritis—such as rheumatoid arthritis, an autoimmune disease, and gout, a metabolic disease—have similar symptoms but are less common.
In This Article:
Shoulder (Glenohumeral) Joint Anatomy and Osteoarthritis
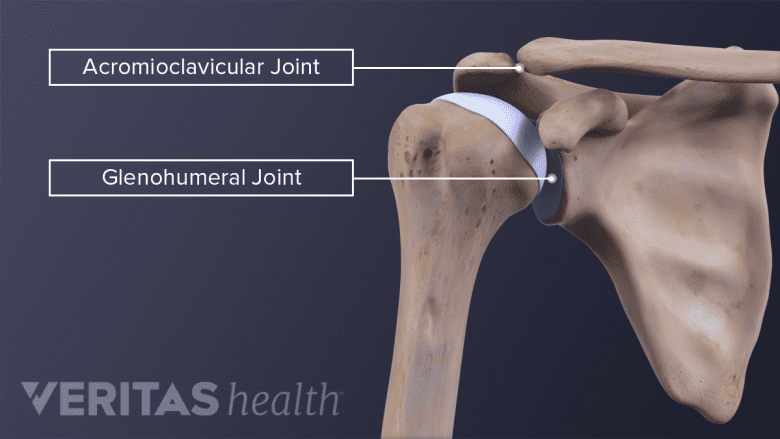
To fully understand shoulder arthritis, it helps to know some shoulder anatomy. The shoulder is comprised of three bones:
- humerus (upper arm)
- scapula (shoulder blade)
- clavicle (collarbone)
The shoulder has 4 joints—places where 2 bones’ surfaces meet—but only 2 of these joints are prone to arthritis and injury:
- The glenohumeral joint is where the rounded head of the humerus nestles into a shallow socket of the scapula, called the glenoid. This ball-and-socket construction allows for the shoulder’s wide range of motion, including circular movement.
- The acromioclavicular joint is located where the clavicle glides along the acromion, which is at the highest point of the scapula. The acromioclavicular joint is more susceptible to osteoarthritis than the glenohumeral joint.
See What Is Acromioclavicular Arthritis (AC Joint Arthritis)?
Glenohumeral joint osteoarthritis is commonly referred to as “shoulder arthritis” and is the focus of this article. The terms “shoulder” and “glenohumeral joint” will be used interchangeably.
How Shoulder Osteoarthritis Causes Pain
The glenohumeral joint may undergo many changes during osteoarthritis process. These changes include:
Damaged cartilage
Strong, slippery articular cartilage lines the surface of the humeral head and glenoid at the areas where they meet. The cartilage helps the bones glide against each other and acts as a buffer to protect the bones from impacting one another. The articular cartilage is naturally thinner in the shoulder joint than in weight-bearing joints such as the knees and hips.
In osteoarthritis, cartilage is injured, worn away, or otherwise degraded. A loss of cartilage can affect the shoulder’s biomechanics. The humerus and glenoid may rub and grind against one another. The bone-on-bone friction can cause shoulder pain.
Bone spurs and other excess bone growth
To compensate for the deteriorated cartilage, the humerus and glenoid may produce excess cells. The cells may form small, scalloped growths, called osteophytes or bone spurs. On the humeral head, bone spurs may form a “goat’s beard” that appears at the bottom of its normally round surface.
These bone changes may result in even more bone-on-bone friction. The shoulder’s range-of-motion may also be affected.
Bone lesions
The bone underneath the damaged cartilage can develop benign (non-cancerous) lesions. These lesions represent areas where healthy bone tissue has been replaced with abnormal tissue. Bone lesions are associated with osteoarthritis pain.1O'Neill TW, Felson DT. Mechanisms of Osteoarthritis (OA) Pain. Curr Osteoporos Rep. 2018;16(5):611–616. doi:10.1007/s11914-018-0477-1. They are not necessarily permanent.
Inflammation
A delicate membrane that surrounds the shoulder joint, called the synovium, can become inflamed during osteoarthritis.
The synovium produces and contains joint fluid, which supplies nutrients to the joint. An inflamed synovium becomes thicker, and the quantity and composition of the joint fluid it produces may change. This potentially painful condition1O'Neill TW, Felson DT. Mechanisms of Osteoarthritis (OA) Pain. Curr Osteoporos Rep. 2018;16(5):611–616. doi:10.1007/s11914-018-0477-1. is called synovitis.
See How Do Synovial Joints Work?
Changes to other soft tissues
When osteoarthritis affects the shoulder’s mechanics, surrounding soft tissues can also be affected. Tendons, ligaments, and bursae may undergo excess strain and friction. Inflammation or injury of these tissues may be a painful side-effect of shoulder osteoarthritis.
For example, as cartilage in the glenohumeral joint deteriorates, the joint space between bones shrinks, possibly putting strain on nearby tendons and causing tendinitis.
Recognizing the symptoms of shoulder arthritis can help lead to an early diagnosis and appropriate treatment. As a general rule, if shoulder arthritis is diagnosed and treated early in the disease process, the patient will experience less pain and fewer long-term complications.
- 1 O'Neill TW, Felson DT. Mechanisms of Osteoarthritis (OA) Pain. Curr Osteoporos Rep. 2018;16(5):611–616. doi:10.1007/s11914-018-0477-1.

