It’s difficult to focus on work or other daily activities when you’re experiencing gout inflammation and pain. Symptoms can last for a few days or even weeks, with the worst pain usually occurring in the first day or two.
While the best thing to do is talk to your physician, there are several steps you can take right away ease your gout symptoms:
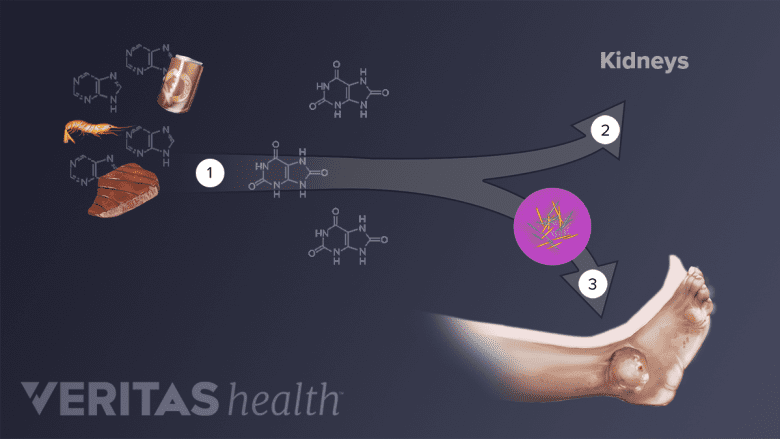
Excess uric acid in the bloodstream can lead to the formation of uric acid crystals in one or more joints, resulting in gout. Read: All About Gout - Symptoms, Diagnosis, Treatment
1. Take an NSAID (but not aspirin)
Over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen, can help relieve gout pain. Avoid aspirin and other medications that contain acetylsalicylic acid, which can make your gout worse.1Ben Salem C, Slim R, Fathallah N, Hmouda H. Drug-induced hyperuricaemia and gout. Rheumatology (Oxford). 2017 May 1;56(5):679-688. doi: 10.1093/rheumatology/kew293 Keep in mind NSAIDs carry potential side effects, such as an increase in blood pressure,2Snowden S, Nelson R. The effects of nonsteroidal anti-inflammatory drugs on blood pressure in hypertensive patients. Cardiol Rev. 2011 Jul-Aug;19(4):184-91. doi: 10.1097/CRD.0b013e31821ddcf4,3Aljadhey H, Tu W, Hansen RA, Blalock SJ, Brater DC, Murray MD. Comparative effects of non-steroidal anti-inflammatory drugs (NSAIDs) on blood pressure in patients with hypertension. BMC Cardiovasc Disord. 2012;12:93. Published 2012 Oct 24. doi:10.1186/1471-2261-12-93 so discuss this treatment with your doctor.
2. Take your prescription drugs
If you've had a gout attack before, your physician may have prescribed drugs to treat attacks. This may be your first line of defense or you may decide to use them only when NSAIDs fail to relieve your pain.
Prescription medications to treat gout include:
- Prednisolone oral tablets, which has been shown to work as well as NSAIDs and often doesn’t cause the same stomach upset. Prednisolone is a type of corticosteroid and does carry other potential side effects, particularly if it is taken for longer than the recommended 5 days.4InformedHealth.org. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Gout attacks: Pain relief. 2015 Mar 11 [Updated 2018 May 17]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK284948/
- Colchicine, which has been shown effective in reducing pain and inflammation if taken in the first 24 hours of an attack. Always follow your physician’s instructions regarding dosing to decrease your risk for potential complications and side effects.
Opioid painkillers, such as codeine, hydrocodone, and oxycodone, are not recommended to treat the pain caused by gout.
See Pain Medications for Arthritis Pain Relief
3. Apply ice to the joint
Cold therapy can offer significant pain relief by decreasing inflammation and dulling pain signals. If this treatment works for you, you can apply the cold pack intermittently throughout the day for 10 to 20 minutes at a time.
See When and Why to Apply Cold to an Arthritic Joint
4. Elevate the joint
Propping up the affected joint can ease pressure and reduce pain. If your big toe is affected (about half of all gout cases affect the big toe), prop it up on a pillow or footstool.
5. Take it easy
Rest the affected joint and keep pressure off it until your pain subsides. Have roomy slippers on hand, so you can keep your feet comfortable until the attack passes.
6. Stay hydrated
Drinking water throughout the day will help flush the uric acid from your system. Aim for drinking 8 glasses a day. Stay away from alcohol and sugary drinks, such as soda and sports drinks, which can make your gout worse.
When medical attention is needed
For severe cases of gout that don’t respond to the treatments above, your physician may recommend corticosteroid injections into the affected joint. Injections can also be useful for people who are sensitive to oral medication.
See Cortisone Injections (Steroid Injections)
Prevent gout attacks
You can help prevent a future gout flare-up by avoiding food and drinks high in purines.
Learn more:
- 1 Ben Salem C, Slim R, Fathallah N, Hmouda H. Drug-induced hyperuricaemia and gout. Rheumatology (Oxford). 2017 May 1;56(5):679-688. doi: 10.1093/rheumatology/kew293
- 2 Snowden S, Nelson R. The effects of nonsteroidal anti-inflammatory drugs on blood pressure in hypertensive patients. Cardiol Rev. 2011 Jul-Aug;19(4):184-91. doi: 10.1097/CRD.0b013e31821ddcf4
- 3 Aljadhey H, Tu W, Hansen RA, Blalock SJ, Brater DC, Murray MD. Comparative effects of non-steroidal anti-inflammatory drugs (NSAIDs) on blood pressure in patients with hypertension. BMC Cardiovasc Disord. 2012;12:93. Published 2012 Oct 24. doi:10.1186/1471-2261-12-93
- 4 InformedHealth.org. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Gout attacks: Pain relief. 2015 Mar 11 [Updated 2018 May 17]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK284948/

