While the basic steps of hip replacement surgery are similar, many variables depend on the patient, the orthopedic surgeon, and the type of prostheses that are used. Below are some common surgical variables patients may encounter.
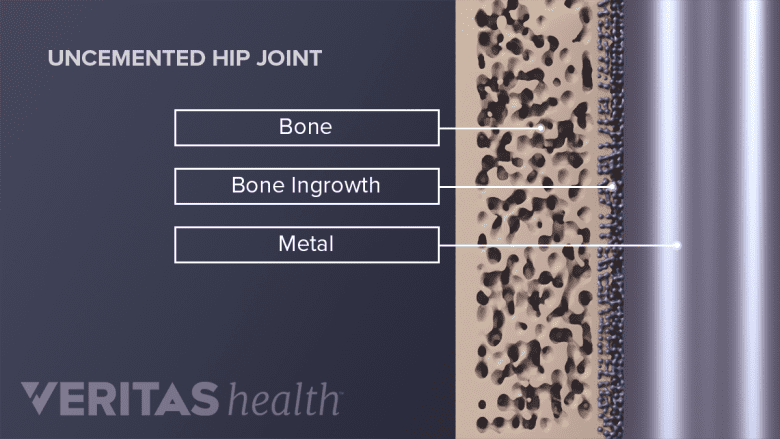
Choosing a cemented vs. uncemented prostheses is another hip replacement factor to consider.
In This Article:
- Total Hip Replacement for Hip Arthritis
- Indications and Eligibility for Total Hip Replacement Surgery
- Total Hip Replacement Surgical Procedure
- Additional Facts and Considerations for Total Hip Replacement Surgery
- Total Hip Replacement Surgery Recovery
- Total Hip Replacement Surgery Risks and Complications
- Total Hip Replacement Surgery Animation
Minimally Invasive Hip Replacement Surgery
Minimally invasive hip replacement surgery is defined differently by different people:
- Some surgeons define it by the actual size of the skin incision, with an incision of 10 cm or smaller indicating a more minimally invasive procedure.1Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321.
- Others define a minimally invasive surgery as one that uses techniques and modified tools to avoid cutting some of the muscle and other soft tissue around the hip. These approaches to the hip are theoretically more “muscle sparing.” (Hip replacement using the direct anterior approach fits this definition.)
See Minimally Invasive Total Hip Replacement
No matter how it is defined, minimally invasive surgery can be technically challenging and pose a unique set of risks. Patients are encouraged to ask about their orthopedic surgeons’ experience. Evidence suggests surgeons who have performed at least 35 to 100 surgeries using a specific surgical method have lower complication rates.2Ravi B, Jenkinson R, Austin PC, et al. Relation between surgeon volume and risk of complications after total hip arthroplasty: propensity score matched cohort study. BMJ. 2014;348:g3284. Published 2014 May 23. doi:10.1136/bmj.g3284,3Hasegawa Y, Amano T. Surgical skills training for primary total hip arthroplasty. Nagoya J Med Sci. 2015;77(1-2):51–57.
Watch Minimally Invasive Hip Replacement vs. Traditional Hip Replacement Animation
Computer-assisted Hip Replacement Surgery
Some orthopedic surgeons use computers during surgery to help ensure optimal placement of the new hip prostheses. Research suggests1Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321. this technology helps ensure:
- Less variability in the placement of hip prostheses
- Better restoration of leg-length and hip joint mechanics
More research needs to be done to confirm these differences and whether they have a long-term impact on factors such as hip pain and how long the artificial hip lasts.1Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321.,4Beckmann J, Stengel D, Tingart M, Götz J, Grifka J, Lüring C. Navigated cup implantation in hip arthroplasty. Acta Orthop. 2009 Oct;80(5):538-44. Review. PubMed PMID: 19916685; PubMed Central PMCID: PMC2823338.,5Gandhi R, Marchie A, Farrokhyar F, Mahomed N. Computer navigation in total hip replacement: a meta-analysis. Int Orthop. 2009 Jun;33(3):593-7. Epub 2008 Apr 3. PubMed PMID: 18386003; PubMed Central PMCID: PMC2903082.
Computer-assisted navigation equipment is costly, and not all hospitals and surgical centers offer it.
Types of Prostheses
The exact design and shape of a prosthetic ball-and-socket can vary. For example:
- The prosthetic ball can range in size, typically 32 mm to 36 mm in diameter.6Tsikandylakis G, Mohaddes M, Cnudde P, Eskelinen A, Kärrholm J, Rolfson O. Head size in primary total hip arthroplasty. EFORT Open Rev. 2018;3(5):225–231. Published 2018 May 21. doi:10.1302/2058-5241.3.170061
- The femoral stem that fits into the femur (thighbone) can be short or long. A shorter stem is about 14 cm long, while a conventional stem can be nearly twice that length.7Mann KA, Ayers DC, Damron TA. Effects of stem length on mechanics of the femoral hip component after cemented revision. J Orthop Res. 1997 Jan;15(1):62-8. doi: 10.1002/jor.1100150110. PubMed PMID: 9066528.
- While the femoral stem is typically made of metal, the femoral head (“ball”) is usually made of metal or ceramic.
Similar types of differences exist among hip socket prosthetics.
There is no definitive scientific evidence showing certain hip prostheses are better than others for all patients.1Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321.,8Rajan Anand, Stephen E. Graves, Richard N. de Steiger, David C. Davidson, Philip Ryan, Lisa N. Miller, Kara Cashman, What is the Benefit of Introducing New Hip and Knee Prostheses? The Journal of Bone & Joint Surgery (Am.), Dec 2011; 93 (Supplement_3); 51-54. doi: 10.2106/JBJS.K.00867 The type of prostheses used will depend on the surgeon’s preference and possibly the patient’s age, anatomy, and lifestyle.
Custom prostheses
Patients may be offered custom prosthetics, tailored to their particular anatomy. Custom prosthetics do not offer notable advantages for most patients.1 They may be appropriate for patients who have rare anatomical differences or certain medical conditions, such as a fractured femur.
Cemented vs. Cementless Prostheses
Another difference among prostheses is how they are attached to the bone. Components may be attached with bone cement or they may be “cementless,” allowing existing bone to grow into them.
In general:
- Cemented prostheses provide more reliable results in people over age 751Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321. or with known osteoporosis.
- Cementless prostheses are used in the majority of hip replacements in the US,9Maggs J, Wilson M. The Relative Merits of Cemented and Uncemented Prostheses in Total Hip Arthroplasty. Indian J Orthop. 2017;51(4):377–385. doi:10.4103/ortho.IJOrtho_405_16 and are particularly favored in younger patients who do not have significant osteoprosis.1Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321.,10Wang T, Sun JY, Zhao XJ, Liu Y, Yin HB. Ceramic-on-ceramic bearings total hip arthroplasty in young patients. Arthroplast Today. 2016;2(4):205–209. Published 2016 Aug 25. doi:10.1016/j.artd.2016.04.004
Keep in mind that each patient is unique, and whether an orthopedic surgeon uses cemented or uncemented prostheses (or a combination) will depend on the surgeon’s preference and the patient’s lifestyle and physiology.
See Cemented vs. Cementless Alternatives in Joint Replacement
The Surgeon’s Experience
One of the most important variables is surgical experience. For example, an experienced surgeon who has expertise in a traditional surgical approach may offer better outcomes than a surgeon who is using the latest technology and methods but has little experience.
- 1 Harkess, JW and Crockarell, JR Jr. Arthroplasty of the Hip. Campbell’s Operative Orthopedics, 13th edition. Philidelphia, PA. Elsevier, 2017: 167-321.
- 2 Ravi B, Jenkinson R, Austin PC, et al. Relation between surgeon volume and risk of complications after total hip arthroplasty: propensity score matched cohort study. BMJ. 2014;348:g3284. Published 2014 May 23. doi:10.1136/bmj.g3284
- 3 Hasegawa Y, Amano T. Surgical skills training for primary total hip arthroplasty. Nagoya J Med Sci. 2015;77(1-2):51–57.
- 4 Beckmann J, Stengel D, Tingart M, Götz J, Grifka J, Lüring C. Navigated cup implantation in hip arthroplasty. Acta Orthop. 2009 Oct;80(5):538-44. Review. PubMed PMID: 19916685; PubMed Central PMCID: PMC2823338.
- 5 Gandhi R, Marchie A, Farrokhyar F, Mahomed N. Computer navigation in total hip replacement: a meta-analysis. Int Orthop. 2009 Jun;33(3):593-7. Epub 2008 Apr 3. PubMed PMID: 18386003; PubMed Central PMCID: PMC2903082.
- 6 Tsikandylakis G, Mohaddes M, Cnudde P, Eskelinen A, Kärrholm J, Rolfson O. Head size in primary total hip arthroplasty. EFORT Open Rev. 2018;3(5):225–231. Published 2018 May 21. doi:10.1302/2058-5241.3.170061
- 7 Mann KA, Ayers DC, Damron TA. Effects of stem length on mechanics of the femoral hip component after cemented revision. J Orthop Res. 1997 Jan;15(1):62-8. doi: 10.1002/jor.1100150110. PubMed PMID: 9066528.
- 8 Rajan Anand, Stephen E. Graves, Richard N. de Steiger, David C. Davidson, Philip Ryan, Lisa N. Miller, Kara Cashman, What is the Benefit of Introducing New Hip and Knee Prostheses? The Journal of Bone & Joint Surgery (Am.), Dec 2011; 93 (Supplement_3); 51-54. doi: 10.2106/JBJS.K.00867
- 9 Maggs J, Wilson M. The Relative Merits of Cemented and Uncemented Prostheses in Total Hip Arthroplasty. Indian J Orthop. 2017;51(4):377–385. doi:10.4103/ortho.IJOrtho_405_16
- 10 Wang T, Sun JY, Zhao XJ, Liu Y, Yin HB. Ceramic-on-ceramic bearings total hip arthroplasty in young patients. Arthroplast Today. 2016;2(4):205–209. Published 2016 Aug 25. doi:10.1016/j.artd.2016.04.004
Editor’s Top Picks
- Total Hip Replacement Surgery Animation
- Cemented vs. Cementless Alternatives in Joint Replacement
- Choosing a Surgeon for Total Hip Replacement Surgery
- All About Anterior Hip Replacement
- Minimally Invasive Hip Replacement vs. Traditional Hip Replacement
- Minimally Invasive Hip Replacement vs. Traditional Hip Replacement Animation

